Pachymeter
(Please scroll down for our product)
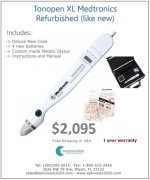
A pachymeter is a medical device used to measure the thickness of the eye's cornea. It is used prior to LASIK surgery, and is useful in screening for patients suspected of developing glaucoma. Modern design incorporates ultrasound technology for measurement of the thickness. Earlier models were based on optical principles.
Until recently, pachymetric measurement of central corneal thickness (CCT) has been the exclusive territory of corneal specialists. After all, is an important tool to evaluate the health of the cornea, measuring its thickness to assess a capacity to pump out excess fluid and maintain clarity. Corneal specialists and general ophthalmologists continue to rely on accurate corneal pachymetry readings to manage patients with corneal ectasias (e.g., keratoglobus, pellucid degeneration, keratoconus), Fuchs’ endothelial dystrophy, bullous keratopathy, corneal rejection post – penetrating keratoplasty, and other causes of corneal edema. However, an increasing number of ophthalmologists are now obtaining CCT measurements on patients with (or suspected to have) glaucoma.
A variety of equipment are available for ophthalmologists
to choose from. The most commonly used equipment uses ultrasound technology
and is the clinical standard. Most of the clinical work studying the association
between CCT and glaucoma has relied on ultrasound pachymetry. Ultrasound
require contact with the cornea; the ophthalmologist delivers a drop of
anesthetic to the eye and applies a sterile pachymeter tip gently onto
the cornea. Ultrasounds continue to be popular, affordable and accurate,
but a newer line of pachymeter that use optical low – coherence
reflectometry technology may enhance accuracy and allow non – contact
pachymetry. Studies comparing optical versus ultrasound pachymetry indicate
that optical pachymetry is at least as accurate as ultrasound pachymetry
when measuring CCT. Some optical instrument even allow real – time
monitoring of measurements. Additional features that ophthalmologists
may consider important when selecting the appropriate equipment, include
portability, ability to communicate with office and surgical equipment
(e.g. excimer laser), and built – in algorithms to estimate the
“true IOP” from a CCT correction.
Please click on the link with the product you are interested or subscribe to our newsletter to receive special promotions.
Accutome |
||
|
|
||
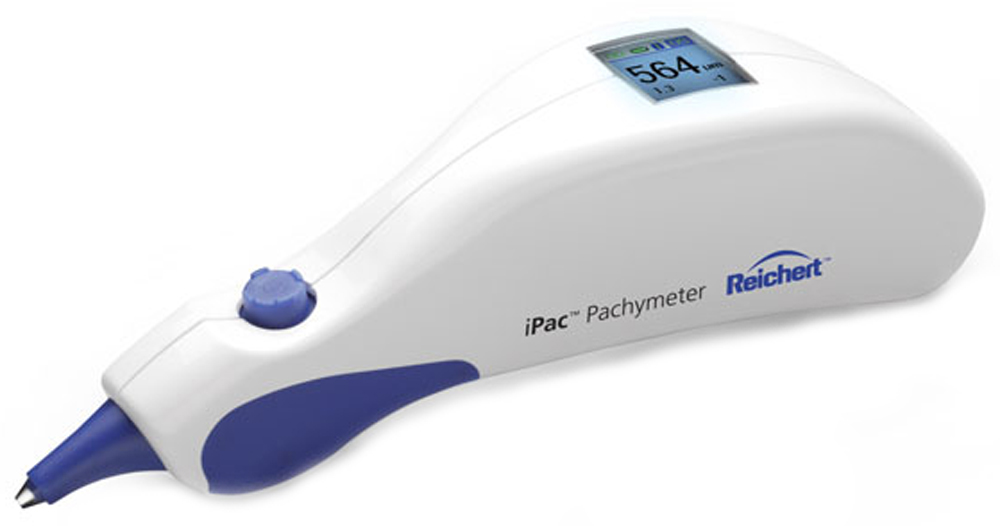
Reichert |
||
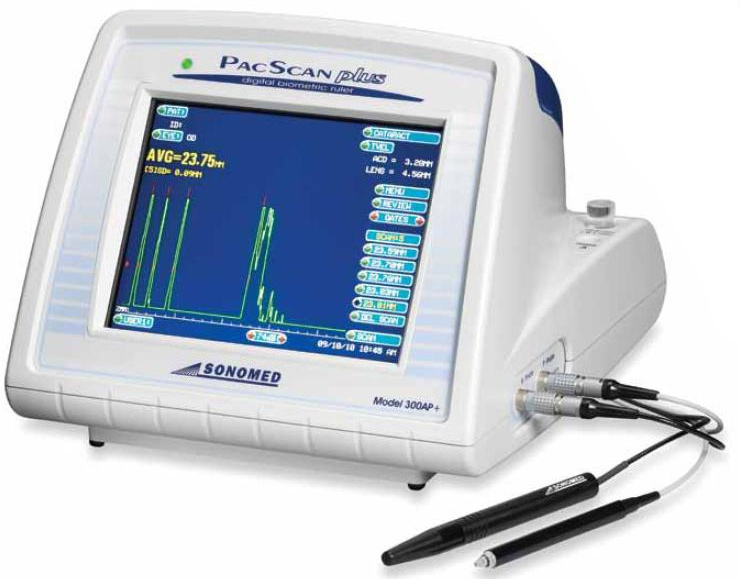
Sonomed |
||
|
|
|
Tomey |
||
|
|
|
|
*only non-USA orders
Done
with Pachymeter ? Return to the Optivision2020 home.
Click here for our Used Equipment Special Sale!
 |
We
accept all major credit cards |
Phone: (305) 593 - 2015
Fax: 1.866.615.2426
Optivision2020, Inc.
3026 NW 79 AVE.
Miami, Florida 33122

Used Marco combo
90 days warranty
Contact us Now